Patient engagement apps often mistake activity for impact, relying on surface-level metrics and feature-heavy designs that don’t translate into better outcomes. The reality is that effective apps are defined by their purpose, shaped by patient behaviour, and built around clear, outcome-driven definitions of success.
Key Takeaways
- Most patient engagement apps are built around the wrong metrics. Downloads and logins feel meaningful but rarely reflect real health outcomes.
- What drives sustained engagement in patient apps isn’t gamification or features, it’s personalization, timely relevance, and showing patients their own progress.
- Defining what success looks like before building a patient engagement app is an important step that many teams skip.
Many healthcare organizations are looking at their patient engagement app from the wrong angle. Downloads, logins, and time-in-app feel like meaningful numbers, but they’re not signals of real patient impact. It’s easy to mistakenly equate engagement with impact, overlooking that a patient’s interaction with a digital health tool alone is rarely enough to drive lasting health outcomes.
The challenge is that “engagement” is not a universal metric. Patient engagement means something different depending on the app, the health condition, the point in the care journey, the outcomes you’re looking to achieve, and what your patients want. If you haven’t defined what success looks like and desired outcomes before you build your patient engagement app, you’re likely to optimize for the wrong thing.
That’s why it’s worth stepping back and getting specific about what success should look like in practice before building an app.
This post covers the counterintuitive truths about what drives sustained patient engagement.
EHR portals: the lowest bar in patient engagement
Before thinking about what good looks like, it’s worth looking at the tools many patients already use. Most major electronic health record (EHR) systems have built-in patient portals. They give patients access to their data, including lab results, appointments, and messages. They’re designed for healthcare orgs to meet their own regulatory and operational needs.
In practice, they were not designed with patient experience or health outcomes in mind. You’re often limited in how much you can customize these built-in patient portals. They offer the same one-size-fits-all interface regardless of condition, care model, or patient need.
They are a clear example of what happens when software developers treat patient engagement as a functional requirement rather than a design challenge.
Custom-built apps win when they’re designed for outcomes, not features
Purpose-built patient engagement apps exist precisely to do what EHR portals can’t, which is deliver an experience designed around a specific patient, condition, and moment in care. But before deciding on features, you need to define what the app is at its core.
Most patient apps fall into one of four categories:
- The app itself is the product and revenue generator
- The app is a companion that enhances, supports, accelerates, and reinforces the main product
- The app is a companion to a service where that service is 1:1 patient care
- The product is actually the data that the app produces
Once you’ve worked that out, you need to consider what outcomes patients are really looking for. This is not what they say in a focus group, but what their behavior tells you when you analyze how they actually use the app.
Real behavior beats wish lists every time. This is why embedding analytics that are compliant with relevant data protection regulations (such as HIPAA) into your product matters.
For example, a remote patient monitoring team recently discovered by analyzing feature usage data and engagement that patients were not checking the app to track their readings, but were looking for reassurance that someone was paying attention. The answer was to build a simple automated message that says: “Your clinician viewed your chart.” That one change, driven by behavioral insight rather than a feature request, drove up sustained usage over time.
The happy abandonment paradox
Sometimes, a patient leaving your app is exactly what success looks like. In one study, the most common reasons for not using or abandoning the mental health app Headspace were that respondents were already using other strategies to support their mental health or no longer needed Headspace.
The researchers noted: “…at some point when people have received sufficient benefits they are likely to stop using a DMHI [digital mental health intervention]”.
This is what researchers call happy abandonment, and it only makes sense if you’ve defined your care model clearly upfront. Here are two examples:
- A chronic disease management app should aim for long-term sustained use
- A post-surgical recovery app has a finite window to work in, and a patient who completes their recovery and moves on is a success story, not a churn statistic
Measuring all of these against the same retention benchmark is a mistake, which is highlighted by the fact that there isn’t even a consistent definition of abandonment, let alone whether it constitutes failure.
The features most teams invest in that don’t move the needle
What works in a consumer app rarely translates directly to a clinical one. It’s easy to look at the gamification mechanics driving retention in fitness or productivity apps and assume the same logic applies to patient engagement, but the context is different. Patients aren’t using your app for entertainment or self-improvement; they’re managing something that matters to their health. Features that work in one setting can create friction or feel patronizing in another.
Apps such as Duolingo on Strava thrive on gamification, competition, leaderboards, streaks, points, badges, and social competition and connection. But these features don’t necessarily work in a digital health app.
Take gamification. A meta-analysis of 79 randomized controlled trials found that engagement improved through reminders and human support, but gamification did not enhance retention.
Welltory, an AI-powered wellness app that has a decade of experience analyzing stress and energy data from over 16 million users worldwide, has also tried gamification as one of its patient engagement strategies, as Asya Paloni, Chief Product Officer at Welltory, was a recent guest on MindSea’s Moving Digital podcast. She explained what features the company has tested to improve user experience and collect better data:
“We tried like little quests, like little health tasks that you had to do every day. Tried streaks. What have we not tried?”
The features that keep patients coming back
The AI-powered CDSS tools that earn adoption share a common trait in that they make the path to a good decision faster without asking clinicians to change how they work. Ambient documentation, inline nudges at the prescribing moment, and clean pre-visit summaries all work because they fit the existing shape of clinical workflow rather than adding to it.
The evidence points to four consistent factors, and none of them are features in the traditional sense.
1. Personalization that reflects where the patient is
Personalization plays a big role in patient engagement. Support that feels tailored, such as coaching or one-to-one messaging, tends to keep people involved and leads to better outcomes than a one-size-fits-all app.
Design features such as personalized messages, chatbots, or avatars can help create that sense of individual attention at scale. They make interactions feel more relevant and timely. However, they don’t fully replace real human support, which most patients experience as more empathetic and trustworthy.
Paloni explains how Welltory does it:
“Give users a small dopamine hit every session with a fresh, personalized health insight. Curiosity brings people back. Guilt doesn’t.“
2. Timely, relevant support tied to real care moments
Generic communication, such as content that arrives on a schedule rather than in response to what a patient is experiencing live, becomes noise quite quickly. Instead, just-in-time adaptive interventions, which deliver context-aware support based on real-time data, consistently outperform fixed-content delivery.
Instead of constant pings, systems can tailor alerts based on what matters to the user, their preferences, how urgent something is, and when they’re available. The aim is to reduce that reflex of swiping things away or hitting snooze.
Simple changes can make a difference. For example, grouping notifications rather than sending them one by one helps keep people informed without the sense of constant interruption, making alerts feel more useful and far less intrusive.
Paloni explains:“Don’t try to motivate people through guilt and performance metrics. Try to focus on relevance.”
3. Showing patients their own progress in terms they understand
When patients can see that something is changing (that their numbers are moving or they’re through a recovery milestone), the app stops feeling like an obligation and starts feeling like evidence that something is working.
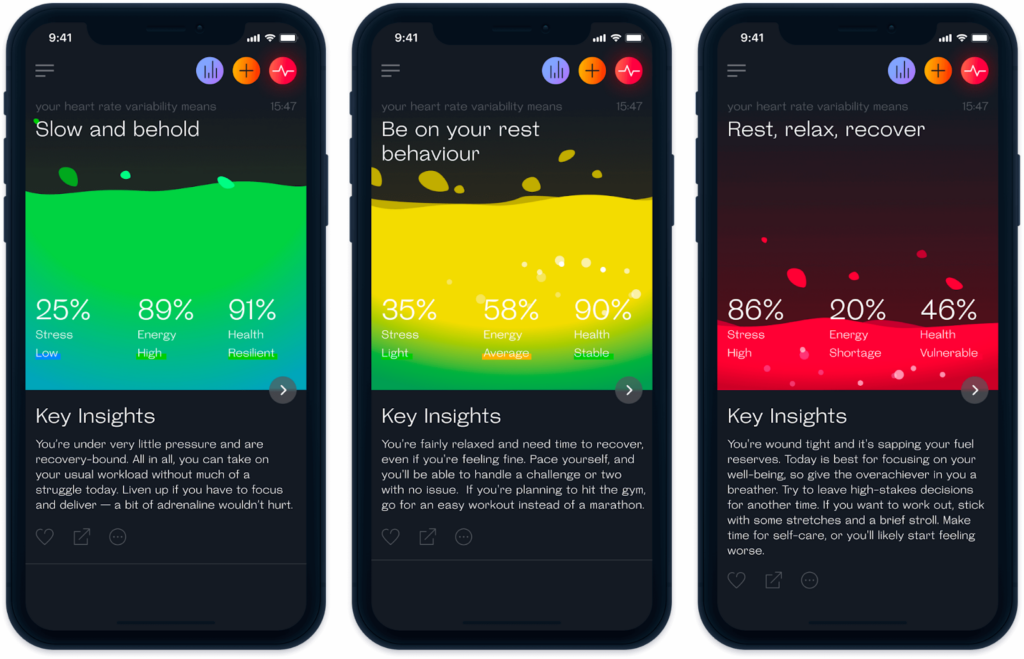
Let’s take Welltory’s approach as an example. Rather than surfacing raw clinical metrics, they translate complex data into animated visual metaphors that patients understand immediately.
“For example, we visualize the state of your nervous system as this liquid that changes shape and color and behavior, depending on what’s happening inside your body,” says Paloni. “Like if the rest and digest part is more dominant and you’re at rest, then it turns into an ocean blue. Or if you’re riled up and stressed, it’s almost like it’s red and bubbling over.”
4. Embedding interventions in platforms that are part of everyday life
A practical way to improve patient engagement is to stop relying on standalone apps and instead deliver support through platforms people already use daily. By embedding interventions into familiar digital spaces, healthcare providers can fit more naturally into existing routines, reduce the effort required to get started, and reach patients who might otherwise disengage.
Messaging platforms are a clear example of how this can work. Services like WhatsApp are already widely used across Asia, Africa, and Latin America, and have been successfully adapted for provider communication, patient education, and public health campaigns.
Because these platforms are low-cost, familiar, and trusted, they make it easier for patients to stay engaged over time, particularly in low- and middle-income settings where traditional digital health apps often struggle to gain traction. For example, an Indian hospital system launched a free WhatsApp channel that provides diabetes education within a platform patients already use daily.
Don’t be afraid to change course
Just because patients engage with your app in a meaningful way today doesn’t mean you can consider the job done. It takes trial and error, built-in analytics, and not being afraid to change things up if the data starts to say something different.
Research suggests that examining app user experience over time is important to identify critical issues at different stages of usage. Users’ needs evolve, and it’s important to keep up with those.
According to Paloni, Welltory has had seven pivots. She explains:
“And I don’t mean minor changes. I mean, like, complete, like, let’s throw everything up and start over. Because behavioral change is so difficult in health…”
Taking a cue from behavioral science
Behavioral science offers a way to improve patient engagement, but it’s often treated as an add-on rather than a foundation.
A useful way to understand engagement is in two layers:
- Micro-engagement: how patients interact with a digital tool, including signing up, logging in, tapping through content, and responding to prompts. This shows they’re engaging with the platform.
- Macro-engagement: how patients engage with their health, such as taking medication, being more active, improving sleep, and following care plans. This is what leads to better outcomes.
High activity in an app doesn’t necessarily mean patients are meaningfully engaged in their care. To improve patient engagement, digital tools need to consider both micro and macro engagements in order to turn in-app interactions into real-world actions.
That depends on thoughtful design and using behavioral science to make prompts relevant, timely, and genuinely helpful.
The questions to answer before you define your feature list
It’s worth being very clear about what you’re trying to achieve before you start pinning down features. The strongest products are built around a clear view of patient needs and the outcomes that matter. Here are some questions to consider before starting with design and build:
What does meaningful patient engagement look like for your population, condition, and care model, and how will you measure it?
For example, in a hypertension app, is engagement defined as daily readings logged, or the sustained reduction in average blood pressure over the past three months?
Are you prioritizing in-app activity, or the real-world health outcomes the app is meant to influence?
For example, should success be measured by weekly logins, or fewer GP visits and improved symptom control?
What is the minimum the app needs to do to deliver value, and where would additional features add friction rather than benefit?
For example, a medication reminder tool that only tracks adherence may outperform a feature-heavy app with coaching and forums that patients rarely use.
Where in the care journey should the app have the greatest impact, and how will that shape its design and functionality?
For example, for post-surgery recovery, is the app most valuable in the first 14 days for symptom monitoring and escalation or for long-term maintenance?
How will the experience be personalized to reflect individual patient needs, including where human support is required alongside digital tools?
For example, a COPD patient with frequent exacerbations might need clinician check-ins triggered by app data, but stable patients may only need automated self-management prompts.
What does success look like over time, and how will you use real-world data to refine and improve the product after launch?
For example, do you expect early engagement spikes to settle into lower but sustained usage, and will you adjust content or alerts based on drop-off patterns?




